
Understanding the Basics of Stress and Vaginal Infections
As we delve into the topic of the connection between stress and vaginal infections, it's important to understand the basics. Stress, a normal part of life, can be both psychological and physical. It's our body's response to any demand or challenge. It's not always negative, as it can help us stay alert and focused. However, prolonged or chronic stress can lead to many health problems, including vaginal infections.
Vaginal infections, on the other hand, are common health issues that affect many women. They occur when the natural balance of organisms in the vagina is disrupted. There are several types of vaginal infections, including yeast infections and bacterial vaginosis, and they can cause a variety of symptoms such as itching, burning, and abnormal discharge.
The Stress Response and Its Impact on the Immune System
The stress response, also known as the 'fight or flight' response, is a physiological response to perceived harmful events, attacks, or threats to survival. This response, while necessary in certain situations, can have detrimental effects on our bodies when it becomes chronic. Chronic stress can weaken our immune system, making us more susceptible to infections, including vaginal infections.
When we're stressed, our bodies produce stress hormones such as cortisol and adrenaline. These hormones can suppress our immune system, impairing its ability to fight off pathogens. This can lead to an overgrowth of bacteria or yeast in the vagina, resulting in infections.
Emotional Stress and Vaginal Health
Emotional stress is a type of stress that is often overlooked when discussing physical health issues. However, it's crucial to understand that our emotional well-being can directly impact our physical health. Emotional stress can trigger a cascade of physiological changes in our bodies, including hormonal imbalances and a weakened immune system.
These physiological changes can disrupt the natural balance of the vagina, leading to infections. In addition, emotional stress can also make it more challenging for our bodies to recover from infections, prolonging the duration of symptoms.
Physical Stress and Its Connection to Vaginal Infections
Physical stress, such as lack of sleep, poor nutrition, and physical overexertion, can also lead to vaginal infections. These types of stress can weaken our immune system and disrupt our body's natural balance, creating a conducive environment for infections to occur.
Physical stress can also lead to hormonal imbalances, which can affect the pH balance of the vagina. A healthy vaginal pH balance is crucial in preventing the overgrowth of harmful bacteria and yeast.
Managing Stress for Better Vaginal Health
Managing stress is not only crucial for our mental health, but also for our vaginal health. Effective stress management can help strengthen our immune system, maintain a healthy vaginal pH balance, and prevent vaginal infections.
There are many ways to manage stress, including regular exercise, adequate sleep, a balanced diet, mindfulness practices, and seeking support from a mental health professional if needed. It's important to find stress management strategies that work best for you and incorporate them into your daily routine.
When to Seek Medical Attention
If you're experiencing symptoms of a vaginal infection, such as itching, burning, abnormal discharge, or discomfort during sex, it's important to seek medical attention. While stress management can help prevent vaginal infections, it's not a substitute for professional medical treatment.
Remember, early detection and treatment of vaginal infections can prevent complications and improve your quality of life. So, don't hesitate to reach out to a healthcare provider if you have any concerns about your vaginal health.
8 Comments
Write a comment
More Articles

Photophobia: Common Causes and Proven Solutions for Light Sensitivity
Photophobia isn't just discomfort in bright light - it's a warning sign of underlying health issues. Learn the real causes, proven solutions like FL-41 lenses, and why skipping diagnosis can be dangerous.
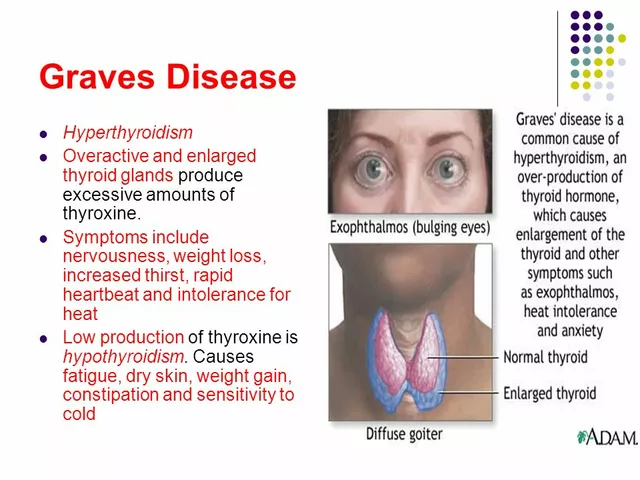
Diagnosing Graves' Disease: Signs, Symptoms, and Tests
I recently learned about Graves' disease, an autoimmune disorder that affects the thyroid gland. The common signs and symptoms include anxiety, weight loss, and a rapid heartbeat. It's important to be aware that some people might experience eye issues like bulging or discomfort. To diagnose this condition, doctors usually perform blood tests to measure thyroid hormone levels, and sometimes they might use imaging tests like ultrasounds. If you suspect you have Graves' disease, it's essential to consult with a healthcare professional to get a proper diagnosis and treatment plan.


joe balak
July 22, 2023 AT 18:17Stress messes with your gut too. Ever notice how your digestion goes haywire when you're overwhelmed? Same thing happens down there. Your microbiome doesn't care if it's work stress or breakup stress-it just knows your body's in chaos.