Wilson’s disease isn’t just a rare liver condition-it’s a silent copper overload that can destroy your brain, liver, and kidneys if left unchecked. It starts with a single faulty gene, ATP7B, which normally tells your liver how to safely get rid of excess copper. When it breaks down, copper doesn’t leave your body. It builds up. Slowly. Painfully. And by the time symptoms show up, damage may already be done.
How Copper Turns Toxic in Wilson’s Disease
Every day, you eat foods that contain copper-nuts, shellfish, chocolate, organ meats. Your body needs a little copper to make red blood cells, connective tissue, and nerve signals. But in Wilson’s disease, the system that controls copper breaks down. The ATP7B protein, made in liver cells, is supposed to load copper onto ceruloplasmin (a protein that carries copper in your blood) and push extra copper into bile so it leaves your body through stool. When ATP7B is mutated, neither of those jobs happens.
At first, your liver tries to cope. It traps copper inside metallothionein proteins, like putting toxic waste in sealed containers. But after years of buildup, those containers overflow. Copper leaks into your bloodstream as free copper-the dangerous kind that isn’t bound to anything. This free copper travels to your brain, eyes, and kidneys. In the basal ganglia (the part of your brain that controls movement), it kills neurons. In your cornea, it forms a rusty brown ring around the iris-called a Kayser-Fleischer ring-that only an eye doctor with a special slit lamp can see. In your kidneys, it damages filtering cells.
Doctors often miss this. Many patients are told they have autoimmune hepatitis because their liver enzymes are high. But in Wilson’s disease, serum ceruloplasmin is usually below 20 mg/dL (normal is 20-50). And your 24-hour urine copper test? It’s often over 100 micrograms-sometimes over 300. That’s not just high. That’s a red flag.
Why Diagnosis Takes Years
One patient in Australia waited seven years before getting the right diagnosis. She had fatigue, joint pain, and elevated liver enzymes. Her first doctor blamed stress. The second thought it was hepatitis. It wasn’t until her 24-hour urine copper test came back at 380 μg that someone connected the dots. That’s not unusual. Surveys show the average delay is 2.7 years. Why? Because Wilson’s disease mimics so many other conditions.
Children under five rarely show Kayser-Fleischer rings. Their ceruloplasmin can be low naturally. Neurological symptoms-tremors, stiff muscles, slurred speech-look like Parkinson’s or even psychiatric disorders. And in low-resource areas, the test for urinary copper or genetic testing might not be available at all. In some countries, patients wait over five years for diagnosis.
That’s why the 2023 updated diagnostic criteria now include genetic testing as a definitive score. If you have two confirmed mutations in the ATP7B gene, you have Wilson’s disease-even if your copper levels are borderline. That’s a game-changer. No more guessing.

Chelation Therapy: How It Works and What to Expect
Once diagnosed, treatment begins immediately. The goal isn’t just to lower copper-it’s to stop it from poisoning your organs before it’s too late. That’s where chelation therapy comes in.
The most common first-line drug is D-penicillamine. It binds to copper in your blood and tissues, forming a compound your kidneys then flush out in urine. Sounds simple, right? But here’s the catch: in 20-50% of patients, especially those with neurological symptoms, penicillamine makes things worse before they get better. Within weeks, tremors can spike. Walking becomes harder. Some patients end up in the hospital.
That’s why doctors now pair penicillamine with zinc. Zinc doesn’t pull copper out-it blocks it from entering your body in the first place. It tells your gut to make metallothionein, which traps copper from food so it passes through you without being absorbed. Zinc is also safer long-term and is often used to maintain control after initial chelation.
An alternative to penicillamine is trientine. It’s just as effective at removing copper but causes fewer neurological side effects. The downside? It costs nearly six times more-around $1,850 a month in the U.S. compared to penicillamine’s $300. Not everyone can afford it. And in Australia, it’s not always covered under the PBS without strict criteria.
Then there’s zinc acetate (Galzin). It’s not a chelator, but it’s the go-to for maintenance. Once copper levels drop, switching to zinc helps keep them there. Studies show 92% of patients on zinc avoid neurological decline as long as their free serum copper stays below 10 μg/dL.
The Hidden Costs of Treatment
Medication isn’t the only burden. Diet matters. You’re told to avoid copper-rich foods: shellfish, organ meats, mushrooms, nuts, chocolate, dried fruit, lentils. That’s not just inconvenient-it’s isolating. One patient on a support forum said, “I can’t eat at restaurants anymore. Even a handful of almonds can send my copper levels up.”
Side effects are common. Nearly three-quarters of patients report them. Nausea. Metallic taste. Mouth sores. Skin rashes. D-penicillamine can trigger lupus-like reactions in 22% of users. Trientine can cause iron deficiency. And if you miss doses? Copper creeps back up. A 2022 survey found 35% of patients regularly skip pills-mostly because the regimen is complex (three times a day, on empty stomach) and the side effects are brutal.
Monitoring is non-negotiable. You need a 24-hour urine copper test every six months. Blood tests for free copper, liver enzymes, and full blood counts every three months. If you’re on penicillamine, you need regular kidney and skin checks. It’s a lifelong commitment.

New Hope on the Horizon
But it’s not all grim. New treatments are emerging. In 2023, a novel copper-binding polymer called CLN-1357 showed an 82% drop in free serum copper in just 12 weeks-with no neurological worsening. That’s huge. Another drug, WTX101 (bis-choline tetrathiomolybdate), got FDA breakthrough status after a trial showed 91% success in preventing neurological damage-beating trientine’s 72%.
And then there’s gene therapy. Early trials are injecting a working copy of the ATP7B gene into liver cells using a harmless virus. In a small 2023 study, six patients showed no serious side effects and improved copper metabolism. It’s not a cure yet-but it’s a path toward one.
Europe already approved a new formulation of tetrathiomolybdate (Decuprate®) specifically for neurological Wilson’s disease because it crosses the blood-brain barrier better than older drugs. The U.S. is catching up.
What You Need to Know Now
If you or someone you know has unexplained liver problems, tremors, or psychiatric symptoms-especially before age 35-ask for a Wilson’s disease screen. Get a 24-hour urine copper test. Ask for ceruloplasmin. Ask for an eye exam for Kayser-Fleischer rings. If you’re on penicillamine and feel worse, don’t stop it-talk to your doctor about adding zinc.
Wilson’s disease used to be a death sentence. Now, with early detection and proper treatment, patients live full, normal lives. The key is catching it before the brain is damaged. The copper doesn’t vanish overnight. But with the right therapy, it stops killing.
And if you’re managing this condition-you’re not alone. There are thousands of people doing the same thing: taking pills on an empty stomach, tracking urine output, avoiding almonds, and fighting to stay healthy. You’re not just surviving. You’re learning how to live with a silent enemy-and winning.
13 Comments
Write a comment
More Articles

Pneumothorax: Recognizing Collapsed Lung Symptoms and Immediate Emergency Care
Pneumothorax, or a collapsed lung, causes sudden chest pain and breathing trouble. Learn the key symptoms, emergency treatments, and what to do after diagnosis to prevent recurrence.
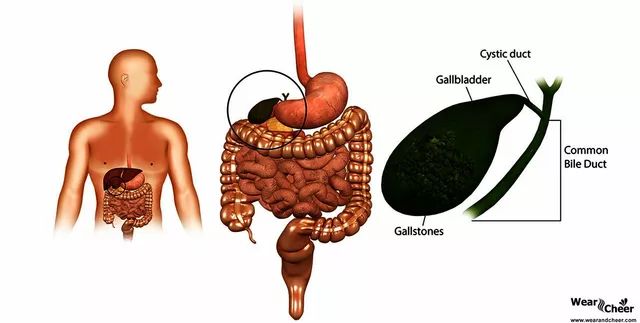
Gallstones and IBS: Understanding the Connection and Managing Symptoms
In my recent research on gallstones and IBS, I discovered that there is a significant connection between the two conditions. Both are digestive disorders and share several common symptoms, such as abdominal pain and bloating. It's essential to understand this link to effectively manage the symptoms and avoid complications. A combination of dietary changes, stress management, and medical treatment can help alleviate the discomfort. Stay tuned for more in-depth information about managing gallstones and IBS in upcoming blog posts.


jobin joshua
November 30, 2025 AT 07:28This is wild 😱 I had no idea copper could do this much damage. My grandma used to make curry with cashews every day... now I'm scared to eat anything 🤯