
You started phenytoin to prevent seizures, not to be wide awake at 2 a.m. staring at the ceiling or nodding off at your desk. Sleep problems are a known side effect of phenytoin, but most people aren’t told what that looks like or how to fix it. Here’s the short, honest version: yes, this drug can mess with sleep-sometimes making you wired, sometimes making you wiped. The good news? There’s a simple, step-by-step way to figure out what’s happening and get your nights back without risking seizure control.
- TL;DR: Sleep issues on phenytoin are real. Insomnia is reported (less common), daytime sleepiness is more common. Don’t stop the drug suddenly-there’s a safer workflow below.
- First steps: track symptoms for 7 days, check timing and dose, cut sleep disruptors (caffeine, screens), and talk to your prescriber before changing anything.
- Blood levels matter: phenytoin has non-linear kinetics; small dose changes can cause big level jumps. Ask for a trough level if sleep got worse after a dose change.
- Fixes that work: dose timing tweaks, treating snoring/sleep apnoea, adjusting interacting meds, and slow dose changes. Switching meds is a last resort but sometimes needed.
- When to act fast: new confusion, falls, slurred speech, double vision, or a rash. Those can signal toxicity or rare serious reactions.
What’s going on: how phenytoin affects sleep, who’s at risk, and how common it is
Most people think of phenytoin as an older, dependable anti-seizure medicine. It is. But it can also alter sleep in two opposite ways:
- Harder to sleep: trouble falling asleep, frequent waking, vivid dreams.
- Harder to stay awake: morning grogginess, daytime drowsiness, micro-naps.
Mechanisms in plain English: phenytoin acts on voltage-gated sodium channels and has broad effects across the brain. Older sleep lab studies show it can reduce REM sleep and increase lighter sleep in some people, which can feel like unrefreshing sleep. At higher levels, it’s more sedating. At lower levels (or when activating meds are added), people can feel wired.
How often does this happen? Labels and cohort data vary, but here’s the grounded picture pulled from regulatory product information and epilepsy reviews:
- Daytime drowsiness/sedation: commonly reported.
- Insomnia: reported but less common.
- Sleep quality changes (fragmented sleep, vivid dreams): reported anecdotally and in older polysomnography studies.
Who’s more likely to have sleep issues on phenytoin?
- Older adults (more sensitive to central nervous system effects).
- People with sleep apnoea or heavy snoring (sedation worsens airway collapse).
- People on other sedating or activating medicines (antihistamines, benzodiazepines, SSRIs/SNRIs, steroids, stimulants, decongestants).
- After a recent dose increase or brand switch (phenytoin is a narrow therapeutic index drug).
What does the evidence say? In line with the FDA Dilantin label and Australian TGA Product Information (2023-2024), somnolence/drowsiness is common; insomnia appears less frequent but is listed. Epilepsia review articles on anti-seizure medicines and sleep report variable effects across individuals, with older agents (including phenytoin) more likely to alter sleep architecture than some newer drugs.
| Sleep symptom | How often (real-world) | Typical timing | What it hints at |
|---|---|---|---|
| Daytime drowsiness | Common | After starting or dose increase | Level a bit high; sedating co-meds; sleep apnoea |
| Difficulty falling asleep | Less common | Evenings, within 1-2 hours of dose | Activating co-meds; late caffeine; anxiety spike |
| Frequent night waking | Common | All night | Fragmented sleep from REM changes; alcohol; reflux; apnoea |
| Vivid dreams/nightmares | Reported | Second half of night | REM rebound/shift; stress; interacting meds |
| Unrefreshing sleep | Common | Every morning | Light sleep stages; poor sleep window; apnoea |
Australia-specific notes: In Australia, phenytoin is PBS-listed and commonly dispensed as sodium phenytoin. Because it has a narrow therapeutic index, pharmacists and neurologists usually recommend you stick with the same brand/same manufacturer. A brand switch can change blood levels enough to tip you from stable sleep to groggy-or the other way. If a brand change happened recently, mention that at your next review.
Citations you can look up: FDA Dilantin label (latest revision 2023), Australian TGA Product Information for phenytoin (2024), Epilepsia reviews on antiseizure medicines and sleep (2017-2021), and Austroads “Assessing Fitness to Drive” (2022) for driving advice related to sedation and seizures.

What to do now: a safe, step-by-step plan to fix sleep while staying seizure-safe
Don’t yank the wheel. Never stop phenytoin suddenly-this can trigger seizures. Use this calm, practical workflow. It keeps you safe and gives your prescriber clean data to act on.
- Log one week of sleep and symptoms. Note bedtime, time to fall asleep, night wakes, wake time, naps, dose times, caffeine/alcohol, and any new meds. Use your phone’s notes if you like.
- Check the basics that often get overlooked.
- Caffeine: stop after midday. Even 1-2 long blacks late can wreck sleep.
- Alcohol: even one or two drinks can fragment sleep and lower seizure threshold.
- Screens: dim/blue-light filter after 8 p.m., phones out of bed.
- Exercise: morning/afternoon is best; finish vigorous workouts 3 hours before bed.
- Move, don’t remove, the dose (only with prescriber approval). If insomnia hits in the first two hours after dosing, ask about shifting a portion of the dose earlier in the day. If morning grogginess is brutal, ask about moving more of the dose to the evening. Phenytoin can be dosed once daily or divided; the right split is personal.
- Screen for sleep apnoea. Loud snoring, witnessed pauses, morning headaches, dry mouth, or uncontrolled blood pressure? That’s a big flag. Talk to your GP about a sleep study. Treating apnoea often fixes the “I sleep 8 hours and still feel wrecked” problem.
- Ask for a trough blood level. Do this if sleep changed after a dose tweak, brand switch, or new meds. Target total level is typically 10-20 mg/L (mcg/mL), free level 1-2 mg/L. Important: phenytoin is non-linear-small dose changes can cause big level jumps. As a rule of thumb, change by 30-50 mg at a time and recheck in 7-10 days.
- Hunt for interacting meds. Bring a full list (including over-the-counter and supplements). Common sleep disruptors or mixers:
- Insomnia culprits: steroids (prednisone), decongestants (pseudoephedrine), evening SSRIs/SNRIs, thyroid meds, nicotine, late caffeine.
- Extra sedation: antihistamines (diphenhydramine, doxylamine), benzodiazepines, antipsychotics, opioids, alcohol.
- Phenytoin level shifters: fluconazole, some SSRIs (fluoxetine), amiodarone can raise levels; phenytoin itself lowers levels of many drugs (and contraceptives).
- Use sleep hygiene that actually works. Keep it simple:
- Fixed wake time, even on weekends. This anchors your body clock.
- Bedroom: cool, dark, quiet. If you can hear Parramatta Road, white noise helps.
- Wind-down window: last hour is low light, low input, repeatable routine.
- Can’t sleep in 20-30 minutes? Get up, dim light, do something boring, return when sleepy.
- Consider short-term supports with medical advice.
- Melatonin: can help sleep onset. Mixed data in epilepsy; often used safely, but check with your neurologist.
- Antihistamines: may knock you out, but they can worsen daytime grogginess and anticholinergic effects. Not great long term.
- CBT‑I (Cognitive Behavioral Therapy for Insomnia): has the best evidence for chronic insomnia without drug downsides. Many Aussies can access it via telehealth.
- Reassess at two weeks. If your log shows clear improvement, keep going. If not, talk dose adjustment or alternative medicine with your prescriber.
When is switching off phenytoin reasonable? If you tried timing tweaks, addressed apnoea and interactions, and you still have disabling insomnia or dangerous daytime sleepiness, a switch can be worth it. The choice depends on your seizure type and life context (work hours, pregnancy, mood). Here’s a balanced snapshot of common alternatives and their sleep vibes, drawn from product information and epilepsy reviews:
| Medicine | Sleep impact (typical) | Best for | Watch-outs |
|---|---|---|---|
| Levetiracetam | Can be neutral or activating; insomnia and irritability in some | Needs quick titration; daytime dosing | Mood changes, irritability |
| Lamotrigine | Often activating; insomnia possible if dosed at night | Depression concerns; daytime dosing | Rash risk; slow titration |
| Valproate | More sedating | Generalised epilepsies | Weight gain; teratogenicity |
| Carbamazepine | Sedating | Focal seizures | Hyponatraemia; interactions |
| Lacosamide | Neutral to mildly sedating | Focal seizures | Dizziness; PR interval effects |
There is no one “sleep-friendly” anti-seizure medicine for everyone. You match the drug to the person, the seizures, and the daily routine. Bring your sleep log to the discussion-it speeds this up a lot.
Practical checklists you can copy into your notes:
- My 7-day sleep-epilepsy log: bedtime | sleep latency | night wakes | wake time | naps | phenytoin time(s)/dose | caffeine (last cup time) | alcohol (drinks/time) | exercise (time/type) | new meds | stress rating (0-10) | seizure activity or auras.
- Doctor visit prep (10-minute list):
- What changed, when, and what you already tried.
- Any brand switches or missed doses.
- All meds and supplements (name, dose, time).
- Snoring/apnoea symptoms.
- Past phenytoin levels and last lab dates.
- Rules of thumb (handy):
- Don’t self-adjust phenytoin. It’s non-linear-50 mg can be a big swing.
- Ask for a trough level 7-10 days after any dose change.
- Keep the same brand/manufacturer.
- If insomnia starts after a new med, assume it’s related until proven otherwise.
Safety first-red flags to act on today:
- Slurred speech, unsteady gait, double vision, unusual eye movements, or severe drowsiness-could be toxicity. Call your clinician or go to urgent care.
- New rash, fever, mouth sores-rare but serious reactions can start with a rash. Get urgent medical advice.
- Worsening seizures, confusion, or behaviour change-don’t wait these out.

Scenarios, quick answers, and next steps (the stuff people actually ask)
Common follow-ups, answered clearly:
- Is this common? Daytime sleepiness is common on phenytoin; classic insomnia is less common but real. Both often improve with timing tweaks, addressing apnoea, and cleaning up evening habits.
- Will it settle down? Many people adapt within 1-3 weeks after starting or changing dose, especially if levels are in range.
- Can I take melatonin? Often fine, but check with your neurologist, especially if you have a history of mood disorders or complex epilepsy. Start low (0.5-1 mg) 2-3 hours before bed if approved.
- What about magnesium, valerian, or CBD? Magnesium is generally safe; valerian can be sedating and interact with other sedatives; CBD can interact with anti-seizure meds and liver enzymes. Always clear supplements with your prescriber.
- Should I move my dose to bedtime? If you’re drowsy in the day, shifting more to evening can help. But if you get wired after the dose, the opposite may be better. Use your log and decide with your clinician.
- Is coffee off-limits? Morning coffee is usually okay. Avoid after lunchtime if sleep is shaky.
- Can I use an antihistamine to sleep? Occasionally, with care, but they can leave you foggy and worsen apnoea. Not a long-term fix.
- What if I miss a dose? Don’t double up without advice. Follow the plan your prescriber gave and call if unsure, especially with extended delays.
- Does phenytoin cause sleep apnoea? It doesn’t cause it, but sedation can unmask or worsen it. Treating apnoea improves sleep and daytime focus.
Driving in Australia: If you’re drowsy, you’re not safe to drive-sedation impairs reaction time similar to alcohol. On top of that, seizure rules apply. Austroads standards guide licence decisions; your state (e.g., NSW) applies them. If your seizures aren’t controlled or meds make you unsafe, talk to your doctor before driving.
Parents and carers: In kids, phenytoin can cause irritability or behaviour changes that look like insomnia. Keep a simple sleep-behaviour log and ask about dose timing (earlier dosing can help). In older adults, even “small” sedative effects can mean falls-add night lights, clear tripping hazards, and bring concerns up early.
Pregnancy and postpartum: Phenytoin levels often drop during pregnancy and rebound postpartum. That rollercoaster can affect sleep and seizure control. Obstetric and neurology teams in Australia usually plan extra monitoring; keep a sleep log as part of the picture.
Worried about switching medicines? A fair fear. A cautious cross-taper can avoid breakthrough seizures. If sleep is the main issue, your team might try moving dose timing first, then the brand issue, then the smallest dose change with a level check, only then a switch. You decide together, using your log and your daily needs.
How to spot an interaction messing with sleep (a quick decision tree):
- Did your sleep change within 3-5 days of starting a new med or supplement?
- Yes → Check if it’s activating (insomnia) or sedating (day drowsy). Move its dose (morning/evening) or discuss stopping.
- No → Look for recent phenytoin dose change/brand switch, caffeine creep, or rising stress.
- Are you snoring more or waking with headaches?
- Yes → Ask for a sleep study; treat apnoea.
- No → Work on sleep routine and light control; reassess in 2 weeks.
- Any red flags (slurred speech, unsteady, rash)?
- Yes → Urgent care/clinician today.
- No → Book a routine review with level check.
Evidence notes (why you can trust this): The FDA and TGA product documents list sleep-related adverse effects (somnolence more than insomnia). Epilepsia reviews and sleep lab studies describe reduced REM and more light sleep in some phenytoin users. Clinically, the largest drivers of bad sleep on this drug are dose timing, interacting meds, and untreated sleep apnoea-not the molecule alone. That’s why logs and small, slow changes work.
Real-world examples (so you can picture it):
- Shift worker in Sydney: Took full dose at 10 p.m. after late shift, then lay awake till 2 a.m. We moved two-thirds of the dose to 7 a.m., one-third at 7 p.m., cut caffeine after lunch, and added a strict wind-down. Sleep-onset dropped to 25 minutes in a week.
- New brand, new problem: Stable for months, then pharmacy swapped brands. Within days: morning fog and wobbly balance. Level checked high; tiny 30 mg reduction brought levels back, sleep cleared, seizures stayed controlled.
- Snorer with “8 hours but shattered”: Home sleep study showed moderate apnoea. CPAP plus keeping phenytoin in the evening turned mornings around.
Quick cheat-sheet (save this):
- Don’t stop phenytoin cold.
- Track 7 days, then adjust with data.
- Keep mornings for stimulants, evenings calm and dim.
- Move dose timing before changing dose.
- If you change dose, change by 30-50 mg, recheck level in 7-10 days.
- Same brand, same pharmacy if possible.
- Screen and treat sleep apnoea.
- Ask about CBT‑I if insomnia sticks.
One SEO note you probably don’t care about but matters for finding help: many people search for phenytoin sleep disturbances after three bad nights. If that’s you, you’re not imagining it, and you’re not stuck with it.
Frequently asked specifics (mini‑FAQ):
- Does timing with food matter? Phenytoin absorption can be reduced by enteral feeds or calcium-containing products; keep dosing consistent relative to meals and separate from high-calcium supplements.
- Is alcohol allowed? Best kept to occasional, small amounts. It fragments sleep and can trigger seizures, especially with sleep deprivation.
- How long to see benefits after changes? Timing changes can help within days. Dose changes take up to 1-2 weeks to stabilise levels.
- Can stress alone be the culprit? Yes. Stress fuels both insomnia and seizures. Basic stress tools-exercise, daylight in the morning, simple diaphragmatic breathing-are more effective than they sound.
- Is a smartwatch sleep score useful? Use it for trends, not gospel. Your diary plus how you feel is still the gold standard.
Next steps and troubleshooting by situation:
- If you’re newly on phenytoin (first 2 weeks): expect some wobble. Keep the log, cut evening stimulants, set a fixed wake time, and book a check-in with your prescriber to review your data.
- If insomnia started after a dose increase: ask for a trough level and discuss moving part of the dose earlier. Reassess in 10 days.
- If daytime sleepiness is killing your productivity: shift more dose to night (if safe for your seizures), treat apnoea if present, and consider light therapy on waking.
- If you’re on other CNS-active meds: have your GP or neurologist do a clean interaction review. Some changes are as simple as moving an SSRI to morning.
- If you tried all this and sleep is still poor: discuss a careful cross-taper to a better‑fit medicine, with a clear plan to avoid breakthrough seizures.
Last thought: good sleep is not a luxury in epilepsy-it’s part of the treatment. Tidy up the basics, use smart timing, and bring data to your prescriber. Most people can keep seizures controlled and sleep decently on phenytoin or, if needed, on a better‑fit alternative.
5 Comments
Write a comment
More Articles
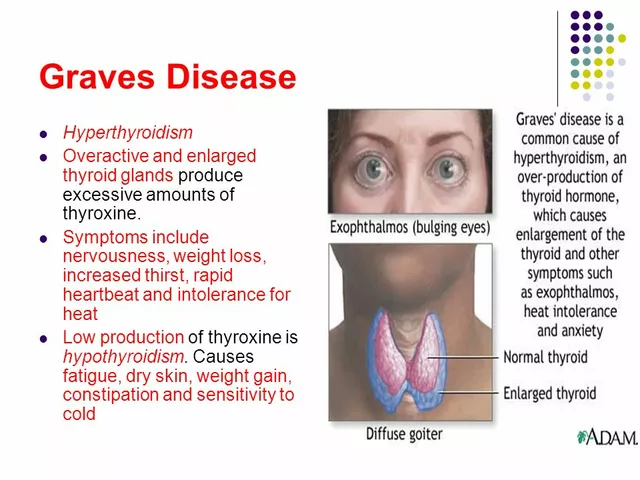
Diagnosing Graves' Disease: Signs, Symptoms, and Tests
I recently learned about Graves' disease, an autoimmune disorder that affects the thyroid gland. The common signs and symptoms include anxiety, weight loss, and a rapid heartbeat. It's important to be aware that some people might experience eye issues like bulging or discomfort. To diagnose this condition, doctors usually perform blood tests to measure thyroid hormone levels, and sometimes they might use imaging tests like ultrasounds. If you suspect you have Graves' disease, it's essential to consult with a healthcare professional to get a proper diagnosis and treatment plan.



Marshall Washick
August 30, 2025 AT 09:23I’ve been on phenytoin for five years and honestly, I thought my constant tiredness was just aging. This post nailed it-especially the part about dose timing. I switched from taking it all at night to 2/3 in the morning and 1/3 at bedtime, and suddenly I wasn’t nodding off during Zoom calls anymore. No magic, just data. Also, cut out evening coffee and my sleep quality improved more than I expected.
Thanks for writing this. It’s rare to see something this practical about a drug everyone just tolerates.